Towards A Truly Paperless NHS
Many organisations have an aspiration to become paperless.
There are huge benefits: for the environment, for efficiency and, these days, for the benefit of service users. When things are paperless, they are generally better, cheaper and faster to use.

Is paperless really possible?
Today, there are a combination of reasons for me to believe that the NHS is truly on its way to achieving its vision to be a paperless organisation. Firstly, it’s now policy. The Five Year Forward View published in 2014 clearly states the ambition for the NHS to be paperless by 2020. The second driver is user demand. Increasingly, patients want to book appointments, check information and communicate with their GPs using digital tools: channels such as Skype, text and screens that give me a real-time view of appointments at my GP’s surgery all help me to better use and plan my time. There is also the huge issue of growing clinical demand. With wearables, data analytics and other digital solutions, we can achieve more proactive management of patients. Checking insulin levels, for example, or monitoring breathing or heart problems remotely all prevent problems escalating and requiring significant NHS resources.
Drivers of change
This year, we’re going to see funding restrictions of £2.5 billion. There is a need to make improvements financially and operationally, the urgency of which was set out in Lord Carter’s 2015 review, Productivity in NHS hospitals. By implementing digital solutions such as cloud, the digital workplace and data analytics, we expect to see major impacts on operational process efficiency. Re-engineering business processes through digital transformation frees up clinicians’ time for frontline patient care – plus, of course, a better patient experience.
Funding support for a paperless NHS
In 2015, the NHS set up Specialist Care Vanguards around key specialisms (cancer, A&E and so on) to remove fragmentation and better target resources. There are also Sustainability and Transformation Plans, with 44 footprints that bring together health and social care and consolidate ‘back-office’ functions such as Procurement, Finance and so on, to drive efficiencies. Then, at beginning of 2016, the Treasury allocated a total of £4.2 billion funding: £1.8 billion to spend on a paperless NHS; £1 billion on cyber security (because you can’t digitise the NHS without addressing cyber-security and data challenges); £750 million on digitising emergency and social care; £400 million on the NHS website, apps, and wifi for patients in hospitals; and £250 million on outcomes and research. This is real, major investment.
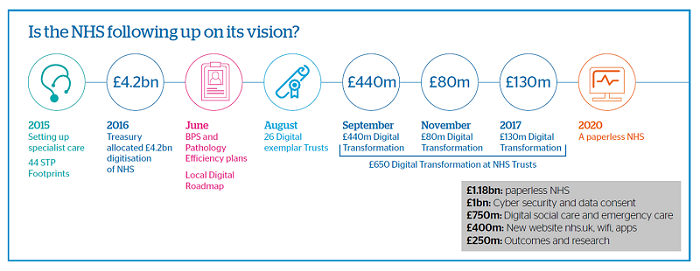
And finally, funding for digital transformation is now allocated locally. There are 16 Global Digital Exemplar Trusts, who each have £20 million to deliver their digital agendas, with a further 20 National Digital Exemplars with a total of £10 million each; plus the £120-130 million for mental health Trusts to digitise their services as global exemplars. Instead of the national initiatives of the past, the NHS is giving accountability, ownership and control to local Trusts. For these reasons, I believe that the NHS paperless digital vision is truly exciting, with momentum and structures for change that I’ve never before seen in my career.
How we can work with the NHS to achieve all this
So, what part does the private sector have to play in all of this? Firstly, we are getting closer to our customer’s customer: the people employed across the NHS and anyone who accesses health services. Digital transformation is an enabler across the health ecosystem. At Atos, we see four main pillars to drive the fundamental transformation that is now needed:
- Integrated care: using digital services to better understand the health economy and deliver more integrated health and social care and improve patient satisfaction
- Collaborative care: using infrastructure and services so that there is collaboration not just within the health and social care economy, but also with patients and their carers
- Mobile care: giving patients ownership and access to their own care plans and records in a way that is convenient for them; and using mobile technologies in care settings to better understand, patient needs and increase clinical resource productivity
- Care analytics: harnessing healthcare data and information to support better-informed clinical decisions, plus wider information on lifestyle and health data to enable clinicians proactively to offer earlier interventions and care.
It is through these drivers that the private sector can work in partnership with clinicians, NHS managers and other partners. Together we can direct and focus resources and expertise to enable the NHS to become a truly paperless organisation that delivers better experiences and outcomes for the 65 million people in the UK who are beneficiaries of its services.